Our experts in the Retina Division treat retina-related disorders and conditions, such as macular degeneration, diabetic retinopathy, retinal detachment, vein occlusion and macularoedema.
Conditions We Treat
The Retina Division provides expert clinical care of retina-related eye diseases and conditions including:
- Age related macular degeneration (AMD)
- Branch vein occlusion
- Central vein occlusion
- Choroidal melanoma
- Choroidal metastasis
- Choroidal neovascularization
- Choroidal hemangioma
- Choroidal nevus
- Diabetic retinopathy
- Epiretinal membrane
- Eye tumors
- Histoplasmosis
- Macular edema
- Macular hole
- Macular pucker
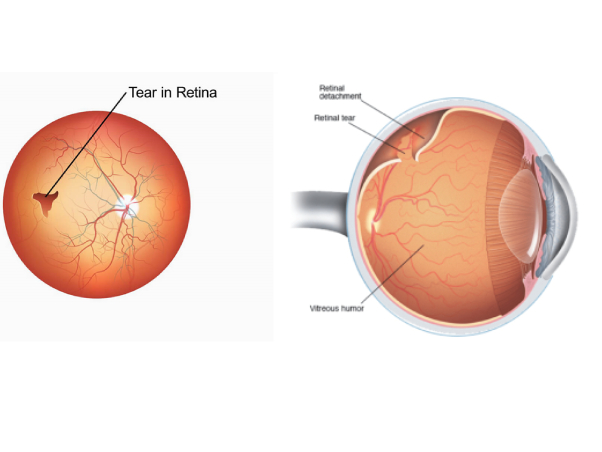
- Retinal detachment
- Retinitis pigmentosa
- Sickle cell retinopathy
- Trauma
- Vein occlusion
- Vitreous hemorrhage
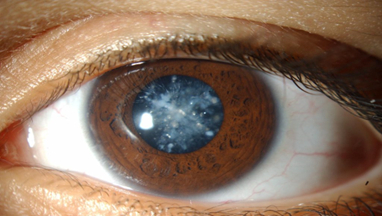
Cataract
A cataract is a clouding of the natural lens of the eye. This clouding of the eye prevents light rays from entering the lens and focusing on the retina. The retina is a light-sensitive tissue lining of the eye and is located at the back of the eye. This cloudiness occurs when some of the proteins from the eye's lens start to alter their shape and obstruct the vision.
There are three basic techniques for cataract surgery
- Phacoemulsification: This is the most common form of cataract removal as explained above. In this most modern method, cataract surgery can usually be performed in less than 30 minutes and usually requires only minimal sedation and numbing drops, no stitches to close the wound, and no eye patch after surgery.
- Extracapsular cataract surgery: This procedure is used mainly for very advanced cataracts where the lens is too dense to dissolve into fragments (phacoemulsify) or in facilities that do not have phacoemulsification technology. This technique requires a larger incision so that the cataract can be removed in one piece without being fragmented inside the eye. An artificial lens is placed in the same capsular bag as with the phacoemulsification technique. This surgical technique requires a various number of sutures to close the larger wound, and visual recovery is often slower. Extracapsular cataract extraction usually requires an injection of numbing medication around the eye and an eye patch after surgery.
- Intracapsular cataract surgery: This surgical technique requires an even larger wound than extracapsular surgery, and the surgeon removes the entire lens and the surrounding capsule together. This technique requires the intraocular lens to be placed in a different location, in front of the iris. This method is rarely used today but can be still be useful in cases of significant trauma.
- cortical cataract
- Diabetic cataract
- Age-related cataract
- Laser cataract surgery
- Femtosecond laser
Cornea Disorders and Treatments
The cornea is the outermost clear, transparent integral layer located in the front of the iris and pupil. It is responsible for the involuntary eyelids reflex and helps to focus the light on the retina. Any change in the cornea layer consistency causes altered vision. With a decrease in transparency of this layer, blurred vision can occur.
Treatments might include medications, laser treatment, or surgery, depending on the condition. Infections are treated with medicated eyedrops (antibiotics, antivirals, and antiparasitics) and, in some cases, oral medication. Herpetic stromal keratitis is a recurring swelling that develops after a herpes eye infection and is managed with anti-inflammatory steroid eye drops.
An abrasion might require temporary patching or a bandage contact lens, depending on the cause and extent of the injury.
- Corneal ulceration
- Corneal transplantation
- Corneal neovascularization
- Corneal degeneration
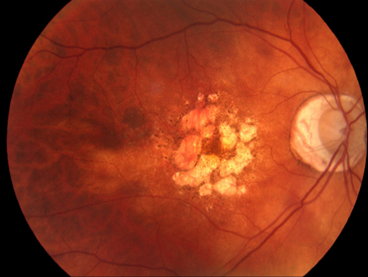
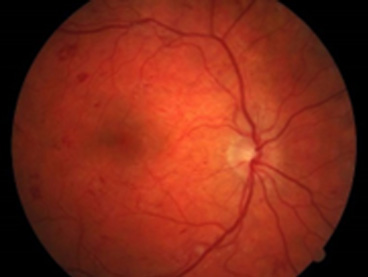
Diabetic Retinopathy
Diabetic Retinopathy (DR) is the leading cause of vision deterioration and blindness across the globe. It is a complication of diabetes affecting the eyes. Among the almost 300 million people who have diabetes, about one-third of them develop Diabetic Retinopathy (DR). Read on to find out what diabetic retinopathy is, its risks and symptoms, whether it is reversible, and how to live with this disease.
- Glycemic control
- Visual impairment
- Advanced diabetic retinopathy
- Diabetic macular edema
- Early diabetic retinopathy
As a common disease afflicting both young and old, diabetes has important implications for the eyes. Fluctuations in blood sugar can cause changes in the focusing of the crystalline lens within the eye and may cause temporary visual blurring, particularly if diabetic control is poor. Diabetes can also cause cataracts in young people, or accelerate the development of cataracts in older people.
Diabetic retinopathy is when the small blood vessels at the back of the eye start to leak or become blocked, and if it’s not detected early, it can cause blindness. Tight control of diabetes can reduce the risk of retinopathy by 60% in type I (insulin-dependent) and 40% in type II (non-insulin dependent) diabetes, and will also reduce the risk of other diabetic complications. When people first develop diabetic retinopathy they exhibit no symptoms, but, if diagnosed at this early stage, it is a treatable condition, which is why it’s important for diabetics to have regular eye tests.
People with diabetes should have an eye examination at diagnosis and thereafter, on a yearly basis by their ophthalmologist.
Pan-Retinal Photocoagulation (Laser)
Laser photocoagulation uses the heat from a laser to seal or destroy abnormal, leaking blood vessels in the retina. The ophthalmologist may make hundreds of laser burns on the retina to stop the blood vessels from growing. Patients may need two or more treatment sessions, which are done as an outpatient procedure.
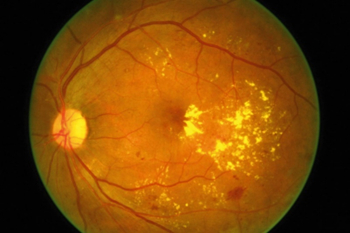
Diabetic Macular Oedema
Diabetics can have leakage at the macular, the central part of one’s eyesight, which usually presents with blurred vision. The ophthalmologist can detect this clinically, by using an optical coherence tomography (OCT) scan of the macular. If the leakage is too close to the central vision, laser is not suitable and the ophthalmologist may suggest an injection of anti-VEGF (protein inhibitors like Avastin or Lucentis for vascular endothelial growth factor) or cortisone into the eye.
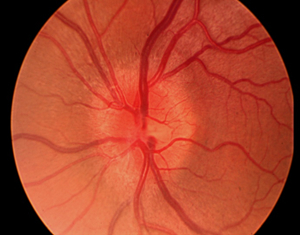
Optic Neuritis
Optic neuritis occurs when the optic nerve, the pathway that transmits visual information to the brain, becomes inflamed, destroying the myelin sheath that surrounds the nerve. Nerve damage that occurs in the section of the optic nerve located behind the eyeball, called retrobulbar neuritis, is most often associated with multiple sclerosis (MS). Optic nerve inflammation and swelling caused by intracranial pressure at the point where the nerve enters the eyeball is termed papillitis. Whilst optic neuritis is most commonly associated with MS, other causes include viral or fungal infections, encephalomyelitis, autoimmune diseases, or pressure on the nerve from tumours or vascular diseases. It is most common in women between the ages of 18 and 40. Optic neuritis usually affects only one eye and may recur several times over the course of years.
Symptoms of optic neuritis include one or more of the following:
- Blind spots, particularly with central vision
- Impaired contrast sensitivity
- Blurred or dimmed vision
- Pain with eye movement
- Sudden colour blindness
- Impaired night vision
- Headaches
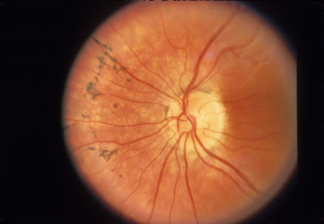
Retinitis Pigmentosa
A group of eye problems that affect the retina, retinitis pigmentosa (RP) is a rare group of hereditary diseases that causes the photoreceptors in the retina to gradually degenerate. People with retinitis pigmentosa lose their vision slowly over time, as it changes how the retina responds to light, making it hard to see.
The type and speed of vision loss from retinitis pigmentosa varies from person to person – it depends on their form of the condition
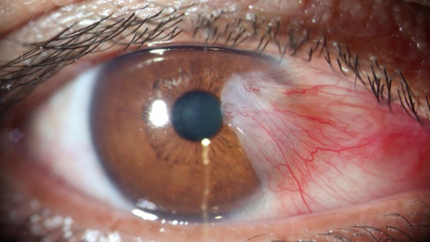
Pterygium Surgery
The term pterygium refers to a fleshy thickening of the conjunctiva which has grown onto the surface of the cornea. Commonly seen in people with high outdoor exposure to UV light, dust and wind, such as fishermen, surfers, and golfers, the treatment of a pterygium is to reduce its exposure to UV with sunglasses or a hat, and to use lubricant eye drops regularly. If the eye becomes inflamed, anti-inflammatory eye drops may be required. If the pterygium continues to grow and threatens vision, or becomes cosmetically unacceptable, it can be surgically removed. The autograft technique, in which conjunctival tissue is harvested from a healthy area and grafted into the defect left after removal of the pterygium, is most commonly used. The graft can be held in place by stitches or a tissue glue (TISSEEL).